Heat Stress vs. Heat Exhaustion vs. Heat Stroke: Know the Difference
Heat Stress vs. Heat Exhaustion vs. Heat Stroke: Know the Difference
Medical and Occupational Health Disclaimer: This article provides general occupational health information based on OSHA, CDC/NIOSH, and clinical guidelines. It is not medical advice and does not substitute for professional medical evaluation, certified first aid training, or emergency medical services. Heat illness diagnosis requires medical evaluation by qualified healthcare professionals. If you suspect heat illness, call 911 immediately. All first aid protocols should be implemented under supervision of trained first aid personnel or emergency medical services. Before implementing any heat prevention program, consult occupational health professionals, safety consultants, and legal counsel.
1. Introduction: Why Distinguishing Heat Illnesses Matters
Every summer in America, workers collapse from heat-related illness. Construction workers, in particular, face staggering risk: they account for 34–39% of all occupational heat-related deaths despite comprising only 7% of the U.S. workforce.1 Yet many of these deaths are preventable—if employers and workers can recognize early warning signs and respond with immediate, aggressive action.
The challenge lies in understanding the spectrum of heat-related conditions. Heat stress, heat exhaustion, and heat stroke exist on a continuum of severity—but they are distinct medical presentations. Workers and supervisors who cannot tell them apart may delay critical intervention, allowing a manageable situation to escalate into a life-threatening emergency. In heat illness, minutes count. The difference between rapid recognition and a 30-minute delay can mean the difference between full recovery and permanent brain damage or death.
This guide explains what these conditions are, how to recognize them, when to call 911, and how to prevent escalation. Understanding these distinctions is not just a medical issue—it’s an occupational safety imperative.
2. The Heat Illness Spectrum: From Mild to Life-Threatening
What Is Heat Stress?
Heat stress is not an illness; it is the condition that creates risk for heat illness. Heat stress occurs when the combination of environmental heat, metabolic heat from work, and protective equipment exceeds the body’s ability to shed heat through sweating and blood flow to the skin.2 In occupational settings, heat stress is measured by the Wet Bulb Globe Temperature (WBGT), an integrated metric that accounts for air temperature, humidity, solar radiation, and wind—not ambient temperature alone.
When workers are exposed to high heat stress without adequate recovery, heat-related illnesses may develop. These range from minor conditions like heat cramps to life-threatening heat stroke.
What Is Heat Exhaustion?
Heat exhaustion is the body’s response to excessive loss of water and salt through sweating. It typically develops after hours of heavy work in heat, when sweating has depleted the body’s fluid and electrolyte reserves.
Workers with heat exhaustion typically show these signs:3
- Heavy sweating (profuse, continued)
- Headache or dizziness
- Nausea or vomiting
- Weakness or fatigue
- Rapid heartbeat
- Possible pale, cool, clammy skin
- Alert mental status (conscious, oriented, may complain of symptoms)
- Core temperature typically below 104°F
Critical distinction: In heat exhaustion, the sweating mechanism still works, and the worker remains conscious and alert. This is the key differentiator from heat stroke.
What Is Heat Stroke?
Heat stroke is a medical emergency in which the body’s thermoregulatory system fails—the cooling mechanism breaks down. The body can no longer control its temperature, and organ damage accelerates minute by minute.
Heat stroke typically presents with these critical signs:4
- Confusion, disorientation, or delirium (hallmark sign of heat stroke)
- Altered mental status or loss of consciousness
- Seizures or convulsions
- Absence of sweating OR minimal sweating (skin may be hot, red, and dry—or paradoxically moist but unchanged in temperature)
- Hot skin (not cooling despite ambient temperature)
- Core temperature typically exceeding 104°F, though diagnosis is based on symptoms, not temperature alone
- This is a medical emergency requiring immediate 911 call and emergency cooling
The defining feature of heat stroke is thermoregulatory failure combined with altered mental status. Unlike heat exhaustion, where sweating continues and consciousness is preserved, heat stroke involves loss of the body’s ability to cool itself and loss of normal brain function.
Side-by-Side Comparison
| Condition | Sweating | Mental Status | Core Temp | Emergency? | Action |
|---|---|---|---|---|---|
| Heat Stress | Increased | Alert & oriented | 37–102.2°F | No (but monitor) | Move to shade; provide cool water; rest breaks |
| Heat Exhaustion | Heavy/profuse | Alert & oriented | <104°F | Monitor closely | Cool immediately (shade + active cooling); give fluids; observe for escalation |
| Heat Stroke | Minimal/absent | Confused or unconscious | >104°F (typically) | YES—CALL 911 IMMEDIATELY | Call 911; begin aggressive cooling immediately (ice bath if available; ice packs if not); do NOT give fluids |
3. Heat Exhaustion: When the Body Starts Losing the Battle
Recognizing Heat Exhaustion
Heat exhaustion is the most common heat-related illness in occupational settings. It occurs when a worker has been losing water and salt faster than they can replace them through drinking and normal electrolyte intake. The worker’s thermoregulatory system is still trying to cool the body through sweating, but the system is becoming depleted.
The key signs are:5
- Profuse, heavy sweating — the body is working hard to cool itself
- Weakness or fatigue—the worker reports feeling exhausted beyond normal work fatigue
- Headache, dizziness, or lightheadedness
- Nausea or vomiting
- Rapid, weak pulse
- Cool, pale, clammy skin (skin is wet from sweat)
- The worker remains conscious and able to communicate
Why this matters: Heat exhaustion is a red flag that the worker’s heat tolerance is being exceeded. If not treated immediately with cooling and fluids, it can escalate rapidly to heat stroke. This is why early recognition and intervention are critical.
Who’s Most at Risk?
Heat exhaustion risk increases with:
- Lack of acclimatization: New workers or seasonal workers returning to heat have 2–3 times higher risk in their first 14 days6
- Heavy physical labor: Metabolic heat production from exertion compounds environmental heat
- PPE and protective clothing: Hard hats, vests, gloves, boots reduce evaporative cooling efficiency
- Inadequate hydration access: Workers unable to drink sufficient water to replace sweat losses
- Inadequate rest breaks: Continuous work without cooling recovery time
- High ambient heat: Outdoor work in direct sun during midday hours
- High humidity: Reduces effectiveness of evaporative cooling
First Aid for Heat Exhaustion
If a worker shows signs of heat exhaustion, immediate action is essential to prevent progression to heat stroke. According to OSHA guidelines, the following steps are recommended:7
- 1. Move the worker to a cooler location immediately: Shade, air-conditioned building, or vehicle. Do not delay.
- 2. Cool the worker actively: Apply cold water to skin; use wet towels; spray with cool water; use fans (only if temperature is below 90°F—fans can worsen cooling in extreme heat).
- 3. Give fluids: Cool water is preferred. If the worker has been sweating heavily for hours, sports drinks with electrolytes can help replace lost sodium. Avoid alcohol and high-sugar beverages alone.
- 4. Monitor continuously: Watch for improvement. Most heat exhaustion victims recover fully within 1–4 hours with aggressive cooling and hydration.
- 5. Watch for progression: If any signs of confusion, altered consciousness, or loss of sweating appear, immediately call 911—this indicates heat stroke escalation.
Key point: Do not assume the worker will recover on their own. Continuous observation is essential. If symptoms do not improve within 1 hour despite cooling and hydration, seek medical evaluation.
4. Heat Stroke: A Life-Threatening Emergency
Critical Signs of Heat Stroke
Heat stroke is a medical emergency. Unlike heat exhaustion, where the body is still trying to cool itself, heat stroke represents failure of the body’s cooling system. The thermoregulatory center in the brain (the hypothalamus) can no longer control temperature, and core body temperature rises unchecked. Simultaneously, the central nervous system begins to malfunction, causing confusion, altered consciousness, and potentially seizures.
Heat stroke signs include:
- Confusion, disorientation, or delirium — This is the hallmark distinguishing feature. The worker may not make sense when speaking, may not recognize familiar people, or may act irrationally.
- Altered mental status or loss of consciousness — The worker may be unresponsive or only partially responsive.
- Absence of sweating in a hot environment — This is paradoxical and critical: the worker’s skin may be hot and dry, or it may be wet but temperature is not dropping.
- Seizures or convulsions
- Rapid, strong pulse (may later become weak and irregular)
- Hot, red skin — The worker’s skin is visibly flushed and hot to the touch.
- Possible loss of consciousness
When in doubt, treat as heat stroke: Not every heat stroke victim will show all these signs, and some may present with only subtle confusion. If a worker is acting confused or disoriented in a hot environment, treat it as heat stroke and call 911 immediately. The cost of unnecessary caution is far less than the cost of delayed treatment.
Why Minutes Matter: The 30-Minute Window
Heat stroke mortality rates illustrate why speed is critical:8
- Untreated heat stroke: Mortality rate 30–80%
- With aggressive early cooling (core temperature reduced below 104°F within 30 minutes): Survival rate 90–100%
This is not a small difference. The difference between rapid recognition and a 30-minute delay can shift outcomes from survival with full recovery to permanent disability or death. Every minute without cooling increases organ damage risk.
The Organ Damage Cascade
Heat stroke is not simple “overheating.” At core temperatures above 104°F, cellular damage cascades across multiple organ systems.9 Heat stroke can cause:
- Brain damage: Direct thermal injury to the hypothalamus (thermoregulatory center), cerebellum, and memory centers. Survivors may experience permanent neurological deficits, cognitive impairment, or movement disorders.
- Kidney injury and acute renal failure: Reduced blood flow during heat stress, combined with myoglobin precipitation from muscle breakdown, can cause acute kidney injury or chronic kidney disease.
- Liver damage: Heat-induced hepatocyte injury and ischemic damage; can progress to acute liver failure.
- Cardiac complications: Dangerous heart arrhythmias, myocardial infarction, or disseminated intravascular coagulation.
- Muscle breakdown (rhabdomyolysis): Releases myoglobin into blood, worsening kidney damage.
- Respiratory failure (ARDS): Inflammatory cascade can trigger acute respiratory distress syndrome.
Long-term consequences: Even with aggressive hospital treatment, 30–50% of heat stroke survivors experience permanent neurological impairment, chronic kidney dysfunction, or other long-term complications.10 This is why prevention is so critical.
5. Why Heat Exhaustion Can Become Heat Stroke
The Escalation Pathway
While heat stress, heat exhaustion, and heat stroke are distinct conditions, untreated heat exhaustion can rapidly escalate to heat stroke. Here’s why:
When a worker develops heat exhaustion, core body temperature is rising, and the sweating mechanism is working but depleted. If the worker is not cooled immediately and hydrated, core temperature continues to rise. At approximately 104°F, the thermoregulatory center in the brain begins to fail. Above this threshold, the body’s cooling mechanisms shut down—sweating stops, peripheral blood vessels constrict, and core temperature rises unchecked. Simultaneously, the central nervous system malfunctions, causing confusion and altered consciousness. Heat stroke has begun.
The critical window: This escalation can happen rapidly—sometimes within minutes. Construction workers who are not recognized as having heat exhaustion and are not cooled immediately may progress to heat stroke while supervisors think they are “just tired” or need to “walk it off.”
Early Intervention Prevents Escalation
The progression from heat exhaustion to heat stroke is preventable with prompt cooling. When a worker with heat exhaustion is moved to an air-conditioned area, cooled with water, and given fluids, core temperature stabilizes, and escalation is prevented. This is why aggressive, immediate cooling is more important than rapid transport to a hospital. On-site cooling can prevent heat stroke from developing in the first place.
6. Risk Factors That Increase Vulnerability
Occupational Risk Factors
Certain job characteristics dramatically increase heat illness risk:
- Outdoor work in direct sun — Especially during midday hours
- Heavy physical labor — Metabolic heat production from exertion; construction, roofing, landscaping
- PPE and protective clothing — Hard hats, safety vests, gloves, boots, respirators. Firefighters in turnout gear face extreme risk.
- Lack of acclimatization — New workers and seasonal workers returning to heat have 2–3 times higher risk in their first 14 days11
- Inadequate work/rest cycles — Continuous work without breaks or cooling recovery
- No shade or cooling areas available — Workers cannot escape heat during breaks
- Time pressure and production schedules — Rush work discourages breaks and hydration
Individual Vulnerability Factors
Some workers are inherently more vulnerable to heat illness:
- Age: Workers over 55 have reduced thermoregulatory efficiency. Paradoxically, very young, fit workers doing intense exertional work can develop heat stroke rapidly without obvious early symptoms.
- Fitness level: Counterintuitively, highly fit workers doing strenuous exertion produce enormous metabolic heat; they may progress to heat stroke without gradual warning signs.
- Prior heat illness: Previous heat exhaustion or heat stroke increases recurrence risk.
- Obesity: Reduced surface area to body mass ratio; reduced cooling efficiency.
- Medications: Stimulants, anticholinergics, diuretics, antihistamines impair sweating or increase metabolic rate.
- Chronic medical conditions: Cardiovascular disease, diabetes, respiratory disease, sleep deprivation—all impair thermoregulation.
- Dehydration at work start: Workers beginning a shift already partially dehydrated face compounded risk.
Environmental Triggers
Heat stress is best measured by WBGT (Wet Bulb Globe Temperature), not ambient temperature alone. WBGT integrates air temperature, humidity, solar radiation, and wind—the true drivers of occupational heat stress.12
OSHA/NIOSH work/rest recommendations based on WBGT:13
- WBGT <82.4°F: 75–100% work allowed
- WBGT 28–84.2°F: 50–75% work allowed
- WBGT 29–86°F: 25–50% work allowed
- WBGT 30–88.7°F: 0–25% work allowed
- WBGT ≥88.7°F: No work recommended
At WBGT ≥88.7°F, outdoor work is not recommended regardless of how acclimated the workers are. This is a critical decision-making threshold.
The “Perfect Storm” Scenario
Heat illness risk increases exponentially when multiple factors combine. The construction industry exemplifies this “perfect storm”: new unacclimatized workers, heavy PPE, extreme heat, inadequate shade, time pressure limiting breaks, and workers who minimize symptoms. This is why construction accounts for such a disproportionate share of occupational heat deaths.
7. First Aid and Emergency Response
When to Call 911: Heat Stroke Red Flags
Call 911 immediately if any of these signs are present:14
- Confusion, disorientation, or delirium
- Slurred speech or difficulty speaking
- Loss of consciousness or unresponsiveness
- Seizures or convulsions
- Absence of sweating in a hot environment (skin hot and dry, or hot and wet but not cooling)
- Any altered mental status or unusual behavior
- Inability to cool down (worker continues to feel hot despite cooling attempts)
When in doubt, call 911 and treat as heat stroke. The cost of unnecessary caution is negligible compared to the risk of delayed treatment.
First Aid for Heat Exhaustion
If a conscious worker shows heat exhaustion signs:15
- Move to shade or air conditioning immediately
- Cool aggressively: Apply cold water; spray with mist; use wet towels; fans (only if ambient temp <90°F)
- Give cool fluids: Water is preferred; for prolonged sweating (>2 hours), sports drinks with electrolytes help prevent hyponatremia
- Monitor continuously: Watch for improvement and for any progression to heat stroke signs
- Continue observation: Recovery typically takes 1–4 hours. Do not assume the worker is safe to return to work without medical clearance if symptoms were severe.
- Watch for escalation: If confusion, loss of sweating, or altered consciousness appears, call 911 immediately
Emergency Cooling for Heat Stroke: The First Priority
For suspected heat stroke, cooling is the FIRST priority—more important than transport to hospital. Call 911 AND begin cooling immediately; do not wait for the ambulance.
According to clinical evidence, cold water immersion is the most effective cooling method:16
- Cold water immersion (ice bath, natural cold water): Cooling rate 0.2–32.6°F per minute. Water temperature 1–62.6°F (33–62°F) is safe and effective; no significant hypothermia risk.
- Ice sheet method (if immersion not feasible): Apply ice packs and cold compresses to major heat loss areas: neck, armpits, groin, chest, abdomen. Cooling rate ~32.3°F per minute.
- Other methods (supplementary only): Fans, evaporative cooling, cold showers are slower (0.01–32.1°F per minute) and should not be relied upon as primary cooling.
Complete heat stroke first aid protocol:17
- Call 911 immediately — do not delay
- Begin cooling immediately while EMS is en route:
- If ice bath available and safe: immerse whole body in cold water (gold standard)
- If not available: Apply ice packs/cold towels to neck, armpits, groin (rapid heat loss areas)
- Remove excess clothing to facilitate cooling
- Continue cooling until EMS arrives
- Do NOT give fluids — Risk of aspiration if unconscious or seizure occurs
- Do NOT move the worker unnecessarily — Limit movement; observe for seizures
- Monitor vital signs if trained
- Inform EMS: “Heat stroke—aggressive cooling in progress. Core temperature needs to be reduced to <102.2°F.”
- Continue cooling during transport — Tell EMS to continue aggressive cooling in the ambulance
- Never leave the worker unattended — Condition can deteriorate rapidly
Critical First Aid Mistakes to Avoid
Common errors in heat illness response can worsen outcomes:
- Not cooling aggressively enough: Providing only shade and cool water is insufficient if core temperature is above 104°F. Active cooling (immersion or ice packs) is essential.
- Using fans in extreme heat: At ambient temperatures above 90°F, fans blow hot air across skin and can increase heat gain. Discontinue fans; use immersion or ice packs instead.
- Giving fluids during heat stroke: Aspiration risk if worker is unconscious or has seizures. Fluids are appropriate only for conscious, alert heat exhaustion victims.
- Delaying 911 call: Heat stroke is a medical emergency requiring advanced life support, IV fluids, and continued aggressive cooling in hospital. Do not delay EMS activation.
- Relying on skin temperature measurement: Standard thermometers (ear, oral, axillary) miss true core body temperature. A worker’s skin temperature of 101°F may have core temperature of 104.9°F. Diagnose by symptoms (confusion, thermoregulatory failure), not by temperature readings.
- Stopping cooling too early: Continue cooling until EMS takes over. Tell paramedics to continue cooling to core temp <102.2°F, as rebound fever can occur.
- Dismissing early symptoms: Heat exhaustion symptoms (“he’s just tired,” “she needs to toughen up”) often precede heat stroke. Take all heat-related symptoms seriously.
8. Prevention: Stopping the Progression Before It Starts
Hydration Management
Adequate hydration is foundational to heat illness prevention:18
- Cool water access: Always available, within reasonable distance, at no cost to the worker
- Drinking frequency: Workers should drink regularly, not just when thirsty. Thirst is a late indicator of dehydration. For moderate activity, ~1 cup (8 oz) every 15–20 minutes; for heavy exertion, up to 32 oz/hour.
- Electrolyte replacement: If sweating will continue for >2 hours, sports drinks with balanced electrolytes (sodium + glucose + water) prevent hyponatremia (dangerous sodium dilution)
- Urine color monitoring: Workers can self-monitor: pale yellow = well hydrated; dark yellow/amber = increase water intake
Work/Rest Cycle Management
Strategic rest breaks in cooled environments prevent core temperature from continuously rising throughout a shift:
- Moderate heat stress (WBGT <86°F): 10–15 minutes rest in shade every 1–2 hours19
- High heat stress (WBGT 30–88.7°F): 30 minutes rest per hour in shaded or cooled area
- Extreme heat (WBGT >88.7°F): Work should not occur, or be significantly reduced with frequent extended cooling breaks
Rest breaks must occur in cooled environments (shade minimum, air-conditioned preferred) to be effective. A worker resting in the sun does not cool.
Heat Acclimatization Protocols
New workers are at 2–3 times higher risk for heat illness in their first 14 days. Acclimatization—gradual physiological adaptation to heat—requires structured exposure:20
- Timeline: 4–14 days of daily heat exposure; minimum 2 hours per day
- Recommended progression:
- Day 1: 20% of normal work duration
- Day 2: 50% of normal work duration
- Day 3: 60% of normal work duration
- Day 4: 80% of normal work duration
- Day 5+: 100% of normal work duration
- Physiological changes during acclimatization: Increased plasma volume, enhanced sweating response, improved cardiovascular efficiency, cellular heat shock protein activation
- Enhanced monitoring required: New workers must be closely supervised during acclimatization. All symptoms should be taken seriously—never dismiss as “just tired.”
Buddy System and Peer Monitoring
Workers observing each other for heat illness signs is a powerful prevention tool:21
- Assign work buddies who stay together and take breaks together
- Buddies watch for symptoms the worker themselves may be minimizing
- Supervisors conduct wellness checks — brief observations for signs of heat illness during work
- Workers trained to self-monitor for symptoms and to report immediately
- Create culture where symptom reporting is encouraged — never penalize workers for heat-related symptoms
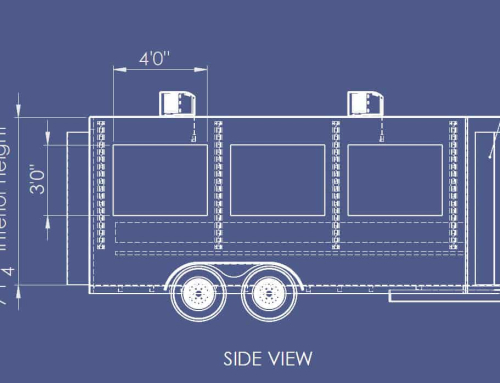
9. The Role of Cool-Down Infrastructure in Prevention
Mobile cool-down trailers and climate-controlled rest environments support multi-faceted heat prevention. While not a replacement for ice bath emergency cooling, on-site cooled environments enable rapid core temperature stabilization during rest breaks and facilitate safe acclimatization for new workers.
Mobile climate-controlled rest areas can:
- Provide rapid thermal relief during rest breaks: A worker with elevated core temperature (103.1°F) entering a 65°F air-conditioned environment experiences immediate temperature differential that initiates physiological cooling
- Support work/rest protocol compliance: Designated cool-down location encourages supervisors to actually schedule breaks (rather than “we’ll cool down when we need to”)
- Enable safe acclimatization: New workers can incrementally build heat tolerance with periodic AC breaks, preventing overwhelming thermal stress
- Reduce cumulative heat stress: Multiple short cooling breaks throughout a shift prevent dangerous core temperature rise that occurs with continuous exposure
Important limitation: Cool-down trailers are prevention and management infrastructure, not emergency treatment. They do not replace ice bath immersion for acute heat stroke. However, for preventing escalation from heat exhaustion to heat stroke, rapid access to cooled environments is a proven, practical strategy. When combined with hydration, work/rest cycles, acclimatization, and training, cooled rest environments fit naturally into comprehensive heat illness prevention programs.
10. Regulatory Context: OSHA and Employer Obligations
Current OSHA Enforcement
As of February 2026, OSHA enforces heat safety through the General Duty Clause (Section 5(a)(1) of the OSH Act), which requires employers to provide workplaces “free from recognized hazards causing or likely to cause death or serious harm.” Heat-related hazards fall squarely under this obligation.22
OSHA’s National Emphasis Program (NEP) on heat, extended through April 8, 2026, prioritizes heat enforcement at high-risk workplaces. Violations commonly cited include inadequate rest breaks, no shade or cooling access, no water, and failure to have emergency response plans for heat illness.
State-Specific Heat Standards
Four states currently have specific, enforceable heat illness prevention standards more stringent than federal requirements:23
- California: Covers outdoor and indoor work at ≥95°F; requires shade, cooling breaks, water, training, emergency response plan
- Oregon: Covers outdoor work at heat index ≥80°F; requires shade, water, acclimatization, monitoring, training
- Washington: Covers outdoor work; requires paid cool-down breaks, shade, acclimatization, emergency response
- Minnesota: Focuses on indoor heat illness; requires written prevention plan, water, cool-down areas, training, acclimatization
If your operations span multiple states, you must comply with the most stringent applicable standard.
Employer Liability for Heat Illness
Employers can face significant penalties for heat-related incidents:24
- Serious violations (General Duty Clause): Penalties exceeding $10,000 per violation
- Willful violations: Penalties significantly higher, up to $160,000+
- Worker’s compensation claims: Heat-related hospitalizations are recordable and can increase insurance premiums
- Fatality reporting: All work-related fatalities must be reported to OSHA within 8 hours
11. Action Checklist for Employers: Implementing Heat Safety
To prevent heat-related illness, employers should:
- ☐ Written Heat Prevention Plan: Document water access, rest break schedule, shade/cooling access, training, acclimatization protocol, emergency response procedures
- ☐ WBGT Monitoring: Use OSHA WBGT calculator or on-site measurement to make work/rest decisions (not ambient temperature alone)
- ☐ Hydration Access: Cool water available continuously at no cost to workers; encourage frequent drinking
- ☐ Work/Rest Scheduling: Implement mandatory rest breaks in shaded or cooled areas based on WBGT thresholds
- ☐ Acclimatization Protocol: New workers follow graduated work schedule (20%-50%-60%-80%-100%) over 4–14 days with close supervision
- ☐ Buddy System: Assign work partners to monitor each other for symptoms
- ☐ Supervisor Training: Supervisors trained to recognize heat illness signs and initiate emergency response
- ☐ Worker Training: All workers trained on heat illness recognition, prevention, and when to report symptoms
- ☐ Emergency Response Plan: Know where cold water immersion is available; have first aid trained personnel on-site; know 911 procedure
- ☐ Cool-Down Areas: Shade minimum; air-conditioned areas preferred for high-heat situations
- ☐ Regulatory Compliance: Consult state OSHA requirements if operating in CA, OR, WA, or MN; ensure compliance with federal General Duty Clause
12. Key Takeaways and Conclusion
Heat stress, heat exhaustion, and heat stroke are distinct medical presentations requiring different responses. The ability to distinguish them—and to respond with appropriate urgency—can save lives.
- Heat stress is the condition; heat exhaustion and heat stroke are the illnesses that result from excessive heat exposure
- Heat exhaustion is serious but manageable: cool immediately, give fluids, monitor for escalation
- Heat stroke is a life-threatening emergency: Call 911 immediately, cool aggressively on-site, do NOT delay emergency services
- The 30-minute window is critical: Reducing core temperature below 104°F within 30 minutes of heat stroke onset dramatically improves survival and reduces organ damage
- Prevention is the priority: Acclimatization, hydration, work/rest cycles, cooled rest areas, training, and buddy system prevent escalation before it starts
- New workers are vulnerable: Provide close supervision during 14-day acclimatization; do not allow them to work full intensity immediately
- Regulatory risk is real: OSHA actively enforces heat safety through General Duty Clause; state standards are often stricter; violations result in significant penalties
For construction site safety managers: Your industry accounts for 34–39% of occupational heat deaths despite being 7% of the workforce. The difference between a near-miss and a fatality often comes down to recognition and immediate response. Train your supervisors to take heat illness seriously. When in doubt, call 911 and cool aggressively. Every minute counts.
Protect your workforce from heat illness with a comprehensive prevention approach: hydration, work/rest cycles, acclimatization, monitoring, training, and rapid access to cool-down environments.
References
- CPWR – Construction Heat Death Statistics
- CDC NIOSH – Heat Stress Overview
- CDC NIOSH – Heat-Related Illnesses
- NCBI/PubMed – Heat Stroke (StatPearls)
- Cleveland Clinic – Heat Exhaustion vs. Heat Stroke
- CDC NIOSH – Workplace Recommendations
- OSHA – Heat Illness First Aid
- PMC – Evidence-Based Heatstroke Management
- Frontiers – How Heatstroke Damages the Brain
- PMC – Heat Stroke to Multi-Organ Failure
- NCBI/PubMed – Heat Illness Overview
- Weather.gov – WBGT vs Heat Index
- OSHA – Water, Rest, Shade Guidance
- PubMed – First Aid Cooling Techniques Systematic Review
- Mayo Clinic – First Aid: Heat Stroke
- OSHA – Heat Standards
- OSHA – Proposed Heat Standard (Federal Register)
- California OSHA – Heat Illness Prevention
- Oregon OSHA – Heat Illness Prevention Rules
- AAFP – Heat-Related Illnesses
- ClimateRig – WBGT Guide
- ClimateRig – Hidden Cost of Heat Stress
- ClimateRig – Heat Stress Deaths & Solutions
- ClimateRig – Monitoring & Prevention Guide
- ClimateRig – OSHA Regulations Guide
- ClimateRig – Cool-Down Trailers Guide
- ClimateRig – ClimateRig Meets OSHA Standards
- ClimateRig – Heat Acclimatization
- ClimateRig – OSHA Work/Rest Cycles
- ClimateRig – OSHA 2026 Guide
- ClimateRig – CellTech Panels Deep Dive
About the author : Stephen
Stephen Allred is a dynamic and accomplished executive with over 20 years of experience in sales and marketing, currently serving as the CMO and CTO of ATS. Renowned for his ability to craft highly effective marketing campaigns, he drives business growth through cutting-edge technology and a results-oriented approach, focusing on high-impact strategies that align with corporate goals while steering clear of ego-driven pursuits. With a deep understanding of customer behavior, Stephen creates compelling campaigns that resonate with consumers, underpinned by the discipline to prioritize the most critical tasks. Boasting over 25 years of management experience, he is a committed leader dedicated to assembling talented teams and unlocking their potential to achieve ambitious objectives. As an adept strategist, he draws on an extensive study of both modern thought leaders and historical figures like Clausewitz and Sun Tzu to devise plans that propel corporate success. A champion of continual learning, Stephen stays ahead of industry trends and fosters a culture of innovation, encouraging his team to think creatively and embrace calculated risks. He graduated Magna Cum Laude from Utah Valley University with a Bachelor’s degree in Finance, where his exceptional performance earned him the prestigious “Outstanding Student Award.”